CPAP Treatment
& CPAP Alternatives

If you have been diagnosed with obstructive sleep apnoea, understanding your treatment options is the first step toward doing something about it.
Two treatments are recognised by the American Academy of Sleep Medicine and the Australasian Sleep Association as frontline options for sleep apnoea - CPAP therapy and oral appliance therapy. This page covers both, along with CPAP alternatives such as surgery and supporting lifestyle measures that may be useful for patients.
CPAP therapy
what is it &
how does it work?
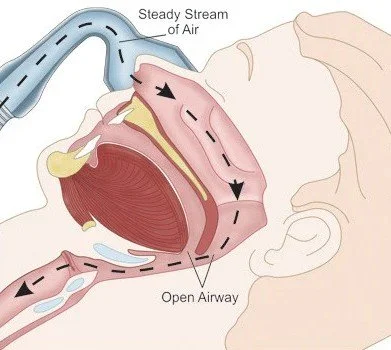
CPAP - continuous positive airway pressure - is the most widely prescribed treatment for obstructive sleep apnoea. A CPAP machine delivers a continuous stream of pressurised air through a mask worn over the nose or mouth during sleep. The air pressure acts as a pneumatic splint - like blowing up a balloon - keeping the upper airway open and preventing the collapse that causes sleep apnoea and snoring.
CPAP is the gold standard treatment for severe obstructive sleep apnoea and is highly effective when used consistently and over 4 hours every night. For patients with significant cardiovascular risk factors - including stroke, high blood pressure, heart disease or diabetes - it remains the recommended first-line treatment.
30–60% of patients prescribed CPAP are unable to tolerate it long-term.
An untreated patient - regardless of the reason they are not using their prescribed treatment - carries the full burden of their condition. This is where oral appliance therapy becomes not just an alternative, but often the treatment that actually gets used.
Why patients may struggle with CPAP
-
Many patients find the CPAP full face mask uncomfortable to wear throughout the night, particularly when changing sleep position. There are other delivery methods too such as the nasal pillows which can be more comfortable than the full face mask. These are not custom made so inevitably there may still be some amount of leakage.
-
The sensation of wearing a sealed mask with supporting head straps can feel restrictive or anxiety-inducing, particularly for first-time users.
-
Even modern, quieter CPAP machines can produce enough sound to disturb both the patient and their partner. Although it must be said that this has come a long way over the years!
-
Pressurised air can cause significant dryness, leading to discomfort, nosebleeds or a sore throat on waking. Dehumidifiers may be helpful but can lead to additional cleaning and CPAP hygiene requirements.
-
Prolonged contact with the mask seal can cause pressure marks, redness and irritation around the nose and face. Supporting and stabilising head straps can also cause some discomfort and chafing with movement and the development of sore spots over time. Speak to your doctor about skin treatment creams which can be helpful to ease these areas.
-
Despite CPAP machines getting smaller as CPAP technology improves, CPAP machines still require a power source, dedicated carry case and airline approval - making travel more complicated.
-
Nasal congestion, hay fever and allergies make CPAP considerably harder to tolerate because the delivery of pressurised air through a blocked nose is uncomfortable, disruptive and often unworkable. The inflammation and swelling of nasal passages as a result of seasonal hayfever or allergies also means that the nasal pillow delivery option may not work well.
Living with CPAP is not always straightforward. Despite its clinical efficacy, CPAP treatment has a well-documented compliance problem. These are the reasons most patients give for finding a CPAP machine difficult to use.
Oral appliances may also be indicated for people with severe OSA who are not compatible with continuous positive airway pressure (CPAP) therapy.
— Australian Dental Association Policy Statement, June 2025
CPAP alternative - oral appliance therapy
Custom oral appliance therapy is the only other scientifically proven frontline treatment for OSA, recommended alongside CPAP treatment by the American Academy of Sleep Medicine and the Australasian Sleep Association.
For snoring and mild to moderate sleep apnoea, oral appliances are the frontline treatment of choice. For patients intolerant of CPAP treatment, oral appliances mean that their OSA can be treated too.
Oral appliances work by gently holding the lower jaw forward during sleep, preventing the tongue and soft tissues at the back of the throat from collapsing into the airway. They are worn in the mouth - similar to a mouthguard - and require no mask, no machine and no electricity.

Oral Appliance therapy
Custom fitted, worn in the mouth
No machine, no noise
Compact and travel-friendly
High long-term compliance
Comparable real-world effectiveness
Can wear with a blocked nose
No electricity required

CPAP treatment
Mask worn over nose or mouth
Requires carry case and power or a lithium-ion battery
Machine required, produces noise
30–60% unable to tolerate long-term
Highest efficacy when tolerated >4hours a night
Difficult to tolerate with a blocked nose
Power source required
CPAP alternatives - what about surgery?
Surgery is rarely a first-line treatment for snoring or sleep apnoea and is generally considered after other evidence-based options - including CPAP therapy and oral appliance therapy - have been thoroughly explored. For snoring specifically, long-term surgical success rates are only 30 to 50%, and procedures carry significant risks including severe post-operative pain, altered voice tone and regurgitation of food.
That said, surgical treatment options for sleep apnoea do exist and for a carefully selected group of patients, they can be highly effective. Soft tissue surgery such as a modified uvulopalatopharyngoplasty (UPPP) procedure aims to reduce upper airway obstruction by reshaping the throat and soft palate. Nasal surgery for sleep apnoea may help where structural nasal problems are compromising airflow and contributing to snoring. Jaw advancement surgery - also known as maxillomandibular advancement or MMA surgery - can significantly enlarge the upper airway in appropriate candidates, though it is a major surgical procedure with a lengthy recovery period.
Hypoglossal nerve stimulation - a newer implanted device that prevents the tongue from collapsing into the airway during sleep - is available for selected patients with moderate to severe obstructive sleep apnoea who have not responded to CPAP. And for patients where excess weight is a contributing factor, bariatric surgery including gastric sleeve and gastric bypass procedures has been shown to meaningfully reduce sleep apnoea severity by reducing the fat deposits around the throat and neck that narrow and collapse the airway during sleep.
Whether surgical treatment for sleep apnoea is appropriate for you depends on your anatomy, the severity of your OSA diagnosis and your individual treatment history. Your GP or sleep physician is the right starting point as they can assess your situation and refer you to the relevant specialist, whether that is an ENT surgeon, maxillofacial surgeon, bariatric surgeon or sleep medicine physician, if surgery is worth exploring as part of your overall sleep apnoea treatment plan.
Lifestyle measures that can help
While lifestyle changes alone are generally insufficient to resolve sleep apnoea or significant snoring, they can meaningfully improve symptoms and enhance the effectiveness of your primary treatment.
-
Excess weight deposits fat in and around the soft palate, tongue and neck structures, reducing the size of the airway. Weight loss can reduce these deposits and enlarge the airway. Although generally beneficial and strongly recommended if there are other weight related health concerns, it is usually not sufficient on its own. Some patients have found weight loss medication to be helpful but it is best to speak to your regular doctor about safe weight loss.
-
Many people have positional sleep apnoea - where sleeping on the back is a key contributing factor. Elevating your head or the head of your bed and avoiding sleeping on your back can make a meaningful difference. Our team can help with practical strategies to encourage side sleeping. There are also other positional therapy aids which may be worth trialing.
-
Nasal obstruction can worsen sleep apnoea and snoring. Simple measures including saline sprays, nasal cones or strips, may not offer a cure for your snoring or sleep apnoea but can enhance the effectiveness of your primary treatment. Steroidal nasal sprays and allergy medication may also be helpful so speak to your GP or pharmacist about these.
-
Alcohol and most sleeping pills relax the muscles of the throat, directly worsening snoring and sleep apnoea. Avoid alcohol for at least four hours before bedtime. Smoking and caffeine can also worsen symptoms by causing swelling of the nasal and throat tissues.
Is a sleep apnoea mouthguard right for me?
Not sure whether oral appliance therapy suits your situation? Our dedicated page walks you through who is most likely to benefit, what the treatment involves and what to expect at each stage.
Are you interested in an alternative to CPAP?
Ready to do something about it?
Book a consultation or a free call with one of our treatment coordinators - no referral needed, no obligation.
Prefer to call us instead?
Our office opening hours are 9am to 5pm Monday to Friday. Thanks for giving us a call. We’d love to speak with you on the phone.
Dedicated.
Involved. Accredited.
Here for you.





